How does the CardioGen-82 work?
CardioGen-82 (Bracco Diagnostic, Inc) is literally the combination of a machine that manufactures a low half-life radioactive tracer, Rubidium-82 (half-life of 76 seconds) from its parent Strontium-82 (half-life of about four weeks) and the Rubidium-82 itself. The FDA terms the machine and the Rubidium-82 combination a “drug” labeled as CardioGen-82.
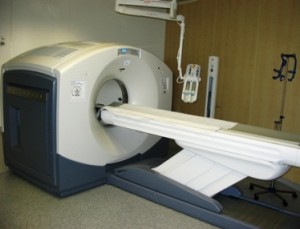
Each time a patient undergoes a Positron Emission Tomography (PET) scan, Rubidium-82 is made “fresh” and on site. Rubidium-82 is made in the machine, by using saline to collect the Rubidium, which then works its way to a receptacle. The operator measures the pharmaceutical’s radioactivity with a dosimeter-like device, and the saline carrying the Rubidium-82 then works its way into a patient syringe. The operator then instructs the computer to have the Cardiogen-82 inject a patient with the radiopharmaceutical. The radioactive Rubidium-82 then works its way through the patient’s circulatory system and through the vessels in the heart. Ultimately a PET camera captures glowing Rubidium-82 enhanced images of the heart, and physicians then interpret where cardiac circulation might be compromised.
In a perfect world, PET scanning using CardioGen-82 is preferred because it is easier to make and use, and more accurate than other methods such as SPECT (Single-Photon Emission Computed Tomography) or N-13 (radioactive ammonia, which has a half-life of 10 days and requires an expensive cyclotron based process to manufacture). However, the complex nature of CardioGen-82, including the way that Rubidium-82 is collected and then injected into the patient necessitates dedicated quality control, technologically advanced operator experience, and great care on the part of the manufacturers, distributors, and end-users of the CardioGen-82.
Recently in June 2011, three patients who had undergone CardioGen PET four months earlier were crossing the Canadian border into the United States and failed a routine Homeland Security radioactivity screening. The screening had become mandatory after the Japanese earthquake, which occurred in March 2011, initiating a tsunami that devastated several Japanese nuclear facilities. After the Japanese tragedy, Homeland Security considered radioactivity screening of international travelers a routine and necessary safety precaution.
After learning that more than one patient had lit up Homeland Security’s Geiger detectors, The FDA issued CardioGen-82 radioactivity danger warnings in July, 2011. Shortly thereafter, Bracco voluntarily withdrew CardioGen from the market, and sent the units for testing to the Los Alamos National Laboratory in New Mexico. At first blush, the FDA attributed the abundance of radioactivity still remaining in the scanned patients, four months after their procedures, as being due to a phenomenon called “breakthrough.”
Breakthrough occurs when the saline being carried through a CardioGen-82 machine contains more of the parent tracer, Strontium-82, than is permissible for use during a CardioGen-82 PET scan. Ideally, if the saline eluate could remove only Rubidium-82, and leave all of the Strontium-82 behind, it would be a perfect world.
How does a CardioGen-82 end user make certain that there is minimum allowable breakthrough during a CardioGen PET? There is an elaborate procedure that has to occur every day before and during use of the machine:
- The user attaches a needle to the end of patient line and inserts the needle into a test vial to collect an eluate sample.
- The computer screen instructs the user to insert the test vial into a vial shield.
- The computer screen then requests the user to start the breakthrough test.
- A subsequent computer screen and a flashing light confirm that the test is in progress (there is an option for the user to abort the procedure).
- The eluate (saline liquid collecting the radioactive Rubidium-82) is diverted from the generator (a tube containing Strontium which has been degrading to rubidium over time) through a waste line and into a waste bottle.
- Then the light holds steady when the eluate is diverted from the generator through the patient line and into the test vial.
- A detector detects a dose rate of 1.0 mCi/sec in the eluate discharged from the generator.
- The light then starts blinking rapidly when the detector measures a peak bolus containing the required radioactivity to perform a scan.
- Upon completion of the elution process for breakthrough testing, the computer shows a time lapse screen, which displays the total time the breakthrough testing has been happening.
- The user then transfers the sample in the vial into a dose calibrator (dosimeter device) to measure the sample’s radioactivity.
- The operator makes note of the time laps indicated on the computer screen.
- Then the operator proceeds to use a data entry screen and enters the time and the radioactivity measurement.
- After the operator enters the data, the computer shows a screen that allows him or her to proceed back to the main menu to perform a system calibration.
- Then the operator starts a second stage of the breakthrough testing.
- In the second stage, the same eluate is measured 60 minutes after measuring it the first time.
- The operator then directs the computer to provide breakthrough results. A screen pops up that includes for reference the previous values that the operator had entered.
- The operator then has to enter the second set of figures taken after a 60 minute interval and the background radiation reading.
- The computer then calculates the breakthrough test results and displays the allowable limits.
- The operator then verifies whether the breakthrough results are within allowable limits, before moving onto patient infusion.
- If the results exceed the limits, a message is displayed by the computer.
- The screen will display a message that the operator should contact the generator manufacturer to obtain a replacement generator.
- In the 60 minute interval between the first and second parts of the breakthrough testing, the operator selects a function from the menu to perform calibration.
- The computer then instructs the operator to insert a new vial, and the patient line should be replaced.
- The operator then proceeds to a screen that displays several data fields.
- The fields are usually preprogrammed with parameters, but the operator has the ability to change them if necessary.
- The operator confirms the parameters are correct and then instructs the computer to begin the calibration elution.
- The computer starts the elution process and indicates that the elution is in progress.
- Once again there is a flashing light during the emptying into the waste bottle and a constant light when the eluate is being transported to the patient line.
- A rapidly flashing light signals that a sufficient bolus is available.
- Time lapse is taken and entered.
- The eluate is placed in a counter to determine radioactivity.
- The user notes the time and the radiation level and enters that information into the proper fields on the computer screen.
- The computer then calculates a calibration coefficient, and presents that as a ration on the screen.
- A desirable range for the calibration ration appears on the computer screen.
- The operator then accepts or rejects the ratio and may instruct the computer to recalculate the ratio
- Then, if all is well, the operator can instruct the computer to inject an automatic infusion of radiopharmaceutical into a patient.
- The system infuses the patient with the radiopharmaceutical and the nuclear diagnostic imaging equipment (a PET scanner) can create an image of the heart of the patient, which has been absorbing the radiopharmaceutical (hopefully, the Rubidium-82 sans an overabundance of Strontium-82).
- If the machine does not contain enough eluant to inject the patient, the computer screen will issue a warning, which includes an option for the user to request another elution.
- If there is still not enough eluant to perform a test, the computer will issue an instruction that no infusion is possible.
- If the infusion begins, the computer will confirm that it is in progress.
- If the infusion has proceeded, the computer will record a summary of the procedure with a patient number attached.
- The information may be transferred to a database via a USB connection.
There are many steps and it takes a long time, even longer if the breakthrough testing procedure has to be repeated because it failed the first time.
Share This


