A Common Fibroid Operation and its Mysterious Link to Uterine Cancer
Dr. Amy Reed is a 41-year-old anesthesiologist in Boston at Beth Israel Deaconess Medical Center. After she underwent a procedure to remove uterine fibroids she was diagnosed with a rare uterine cancer and was told that a minimally invasive procedure called morecellation may have spread her stage IV cancer.
A draft article to be published in the New England Journal of Medicine (NEJM) calls for a moratorium on morcellation, commonly used during a hysterectomy to remove common growths in the uterus called fibroids.
The surgery involves grinding up the fibroids and removing the pieces through small incisions. Dicing the growth up before removal may inadvertently be spreading cancerous material through the abdomen, according to the draft article. Dr. Reed’s husband, a Boston area surgeon, has launched a campaign to immediately halt the procedure.
His petition says one in 415 women who undergo fibroid surgery actually have a sarcoma. That translates to two to five women who may have cancer spread by a morcellation procedure.
You’ve heard the term “minimally invasive” before. Johnson & Johnson’s Ethicon division dubbed transvaginal mesh and its implant procedure as “minimally invasive.” It is not a coincidence that the main surgical tool used in morcellation is made by Ethicon.
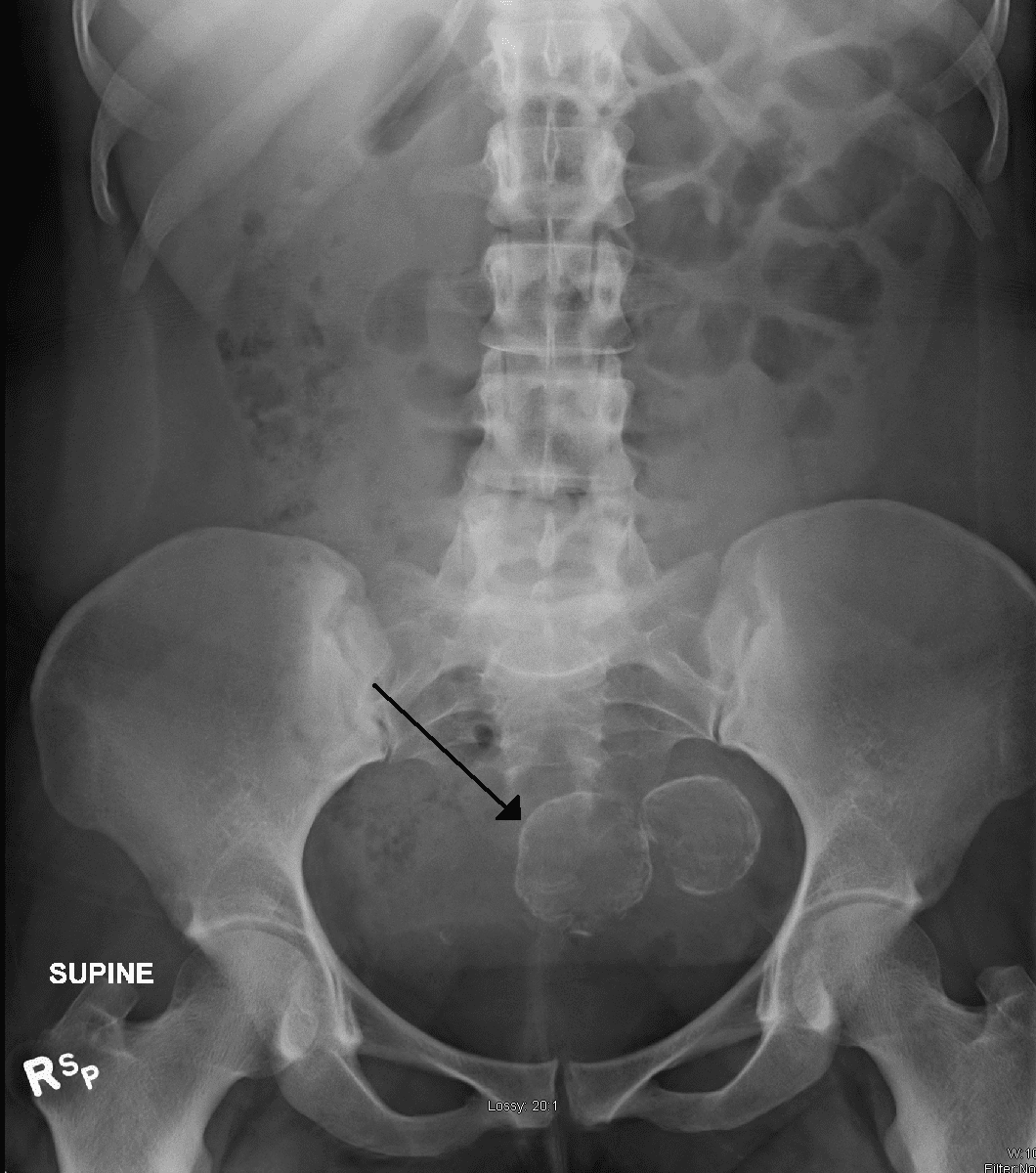
Fibroid development is very common in 20 to 40 percent of women over the age of 35. A fibroid is a growth made of muscular tissue of the uterus and often is benign but fibroids can mask a cancer growth. Often doctors remove what they believe to be a fibroid and never have a test to determine if cancer was present.
Over the last 10 years, the open abdominal surgical operation option has declined in favor of “minimally invasive” techniques involving laparoscopic and robotic surgery and so has morcellation.
The American Congress of Obstetricians and Gynecologists (ACOG) reports of the nearly 500,000 hysterectomies done in the U.S. in 2010, about 11 percent involved morcellation and that number is considered to be conservative.
A study out of Boston one year ago found a nine-fold higher risk of uterine cancer than was being quoted to patients. A South Korean study found the rate of one of the deadliest forms of uterine cancer, leiomyosarcoma, was twice as high after tumors were removed via morcellators than for those whose tumors were removed intact. As far as Dr. Reed, she reportedly faces an up to 80 percent chance her cancer may have spread to her abdomen. She blames the hospital, not for her cancer, but for making it worse.
For now, Massachusetts General Hospital, affiliated with Harvard University, will tell women about the higher risks from the technique and Brigham and Women’s Hospital will limit the procedure.
Share This