If you are a user of bisphosphonate drugs – be a very active participant in your therapy; do periodic research; ask questions; and demand reasonable answers.
An advisory panel to the Food & Drug Administration has recently taken action on the danger presented by drugs such as: Actonel, Fosamax and Boniva. These are drugs originally marketed by Merck (Fosamax) and prescribed for people suffering from osteoporosis. Sadly, the decisive action the committee panelists decided to take was to affirmatively do nothing. So, unless the FDA itself acts to strengthen warnings or information provided to patients at the time these drugs are prescribed, it will require vigilance on the part of patients to protect themselves.
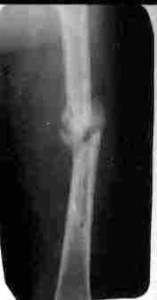
Osteoporosis is a thinning of bone tissue and a loss of density in bone that usually develops over time. It is the single most common form of bone disease known. Ironically, bisphosphonates have been found by a number of researchers to cause atypical thigh and jaw fractures in patients taking them. This is particularly remarkable after patients have been taking the drugs for around five years or more.
One of the members of the advisory panel, Lewis Nelson, director of medical toxicology at New York University, said, “…be very clear that efficacy may fall off after a period of time, perhaps five years. Serious concerns have been raised about risk, and those need to be continually evaluated as well.”
Bisphosphonate sales has been a huge money maker for pharmaceutical companies:
- Fosamax’s, Merck, reached sales as high as $3.19 billion in 2005 before other maker’s products sharply reduced those yearly sales.
- Actonel’s maker, Warner Chilcott had 2010 sales of $579 million.
- All together bisphosphonate sales generated $4.2 billion in the U.S. and $7.6 billion in sales worldwide during 2010.
Merck ten year clinical studies demonstrate that Fosamax’s benefits outweigh its potential hazards to osteoporosis patients – there is a big surprise.
In a 17 to 6 vote, some panelists felt new, stronger warnings should be provided to patients. Other panelists felt there was insufficient data to warrant stronger warnings than already exist.
Dr. Jennifer P Schneider has a little different view. She was taking bisphosphonate drugs for osteoporosis, but was otherwise a completely healthy woman, when her femur fractured as she was simply standing and waiting for a New York subway train. She sets forth:
What should we advise our patients? Bisphosphonates are stored in bone for up to 10 years after their consumption is stopped, although their metabolic effects are of shorter duration. Studies have shown the efficacy of bisphosphonates in the first five years of therapy in improving bone density and diminishing the risk of fractures. After that, until additional studies are done that clarify the risks of non-traumatic fractures and delayed healing in patients on long-term bisphosphonates, and which risk factors, if any, can help predict which patients are at increased risk of these adverse events, it is reasonable to suggest to patients to stop the drug after several years, continue weight-bearing exercise and calcium, and wait to see what the next scheduled DEXA scan shows.
Share This